News
How Ethical Would An Ebola Vaccine Be?
The Ebola virus has now claimed over 3,000 lives, according to the World Health Organization, and shows no signs of slowing. Since it first emerged in March of this year, 6,574 cases have been reported, and an unrelated outbreak in the Democratic Republic of the Congo has killed another 42 people. With death tolls increasing day after day, the need for a vaccine is at an all-time high, but scientists are now debating the ethical dilemmas of an Ebola vaccine that will not have undergone the testing that is normally required for these types of drugs. But time is of the essence, now more than ever.
American and international doctors are moving full speed ahead in attempts to produce a vaccine or a cure for the virus in what seems to be a race against time. The total number of cases expected by November now stands at 20,000, which was previously the figure projected as the total over the next nine months. But with the number of cases doubling every few weeks, the need for a cure is growing more and more critical every day.
Unprotected and unprepared
According to Dr. Joia Mukherjee, the chief medical officer of Partners in Health, without a way to treat the disease, Liberia, one of the hardest hit countries, has seen a "general collapse of the health care system." Mukherjee continued, "...Physicians and nurses and other health workers are staying home. They feel unprotected and unprepared to deal with this — and they are."
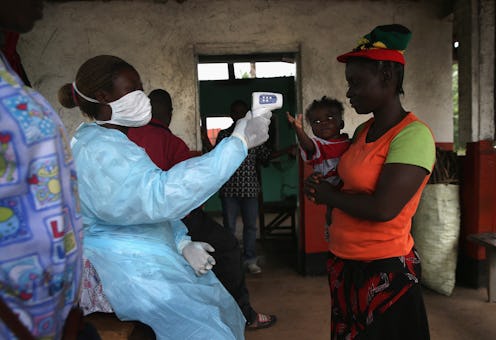
And even with doctors and healthcare workers attempting to abide by the strictest of heath code protocols, like donning protective wear and quarantining sick individuals, the disease continues to spiral further out of control.
A rush for drugs
As such, it comes as no surprise that the attention of the world has now been fixed upon pharmaceutical companies like GlaxoSmithKline (GSK) and Johnson & Johnson, who face increasing pressure from the US Centers for Disease Control and Prevention as well as the international community to come up with solutions to the virus. And happily, it seems that some vaccines will be ready for distribution by the year's end.
This expedience is largely due to the WHO's agreement to forego the normal clinical trial and experimental phase and move directly into treatment. With the growing panic and state of emergency surrounding Ebola, this seems all but necessary. This means that some patients may be receiving relatively untested drugs, and will be serving as human guinea pigs for a potential solution.
But the particulars of how this nearly unprecedented dismissal of safety and testing protocols have yet to be determined. Adrian Hill, a GSK employee who is conducting safety trials on healthy volunteers of an experimental Ebola shot told Reuters, "Nobody knows yet how we will do it. There are lots of tough real-world deployment issues and nobody has the full answers yet."
Ethical dilemmas
This, of course, has raised significant ethical concerns from the scientific and medical community. "Normally safety is the absolutely paramount thing when you're developing a new vaccine, but this time we're going to have to take more risks," Brian Greenwood, a professor at the London School of Hygiene and Tropical Medicine said in an interview with Reuters. But beyond the safety issues, a drug's effectiveness can often only be told through time, which means that foregoing the testing phase of some of these treatments may result in the production of drugs that don't actually do anything for Ebola at all.
To address some of these questions, as well as other practical and ethical dilemmas that a potential Ebola vaccine will bring, the WHO has called a meeting amongst vaccine specialists, epidemiologists, pharmaceutical companies and ethicists to take place on Monday and Tuesday.
Part of the problem, many say, is the fact that scientists are trying to create a vaccine for a disease that is running rampant, creating chaotic situations in areas that need treatment the most. This means that developers are charged with doing two things at once, evaluating and deploying a vaccine simultaneously, when normally there is a clear order in which treatments are first examined then distributed.
But now, doctors may need to go forward with medications even before they are proven safe and effective. And the troubles are compounded by the fact that it will be difficult to measure the success of a drug in areas where sanitation and contamination are huge issues. For example, while Dr. Kent Brantly and Nancy Writebol survived their Ebola infections after receiving doses of ZMapp, an experimental drug, a Liberian doctor who took the same medicine died in spite of the treatment. So was it the fact that Brantly and Writebol were treated in the much less crowded, much cleaner and well-prepared facilities in the United States that made a difference, was it ZMapp itself, or was it something else entirely?
did it work?
The same issue will likely arise with any other experimental treatment. Doctors will be unable to tell whether a drug's effectiveness (or ineffectiveness) is due to the treatment or external conditions. Moreover, it may be unethical to test a drug using a control group, which is normally how clinical trials are done. As Hill told Reuters, to "do a trial where some people don't get the vaccine because they are in the control group...especially if you have reasonable evidence that the vaccine might work" wouldn't be ethical.
But despite the ethical and moral concerns, one thing remains clear — something must be done about Ebola. And as Peter Piot, a co-discoverer of the Ebola virus in 1976 and now director of the London School of Hygiene and Tropical Medicine told Reuters, "It may be that without a vaccine, we can't really stop this epidemic."
Images: Getty Images (5)