Life
HIV-Preventative Medication Keeps Going Up In Price — Here’s Why It Matters
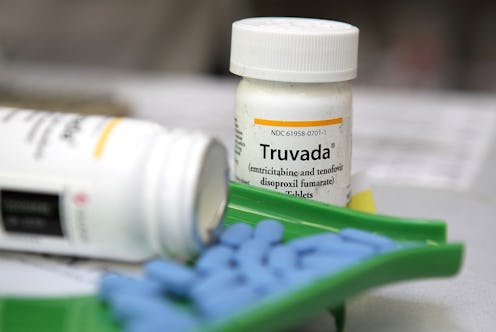
Pre-exposure prophylaxis, or PrEP, an HIV-preventive drug that helps protect those most at risk of infection, has been a game-changer in terms of HIV prevention in recent years. But while the drug has the potential to dramatically curb HIV infections on a global scale, rising PrEP costs mean that it’s often inaccessible to those who need it most.
Quinn Tivey, a representative for The Elizabeth Taylor AIDS Foundation and the actor's grandson, tells Bustle via email that PrEP medications are a powerful “means of [HIV] prevention, with the ability to reduce the risk of HIV transmission by up to 99 percent.” And considering that in the United States, HIV disproportionately affects low-income populations and those without easy access to health care, PrEP access is crucial for protecting populations most at risk of HIV infection. The World Health Organization (WHO) reports that approximately 36.9 million people worldwide were living with HIV at the end of 2017, though these numbers vary region to region across the globe. In the United States alone, it’s estimated that 1.1 million people manage HIV, per the Centers for Disease Control and Prevention (CDC).
According to NPR, in a nationwide effort to halt HIV infection, steps are being taken to expand access to PrEP. But public health officials face some pretty formidable challenges in the process. Increasing PrEP prices — like Truvada’s jump in cost by 45 percent within the last six years, as NPR reported — mean that the drug is often pushed out of reach for those most at risk of infection. Despite the fact that most insurers cover PrEP, steep pricing means that remaining out-of-pocket costs for patients can be overwhelming. NPR reports that the list price for a 30-day supply of PrEP carries a price tag of around $2,000.
Per the CDC, studies show that PrEP is about 90 percent effective when used as directed. The CDC also notes that PrEP must be taken daily in order for it to work. Access to both HIV preventative drugs like Truvada, and treatments for those managing HIV long-term, can be lifesaving. “Today, people can live long and very healthy lives with HIV, [which was] unheard of at the beginning of the epidemic,” Tivey says. In order to continue making such progress, however, HIV-preventive measures like PrEP are essential.
NPR also reports that Truvada's manufacturer, Gilead Sciences, is making assistance programs for the uninsured and underinsured more widely available. Gilead spokesperson Ryan McKeel told NPR that “we have designed our assistance programs with the intent that people can benefit from their full value, [but] we cannot control the actions or decisions of health insurers.” McKeel also told NPR that Gilead funds advertising, like TV and print ads, to reach those most in need of PrEP.
Despite these efforts, “Cost and access are [persistent] barriers to [PrEP] use, but so are awareness and stigma,” Tivey says. In order to overcome these obstacles, Tivey stresses that “compassionate communication,” at both the peer and community levels, are key to expanding both awareness of HIV prevention, and access to prophylactic methods like PrEP. In order to protect against potential HIV infection, Tivey further emphasizes the importance of education, personal empowerment, and overcoming stigma in the effort to prevent HIV. “Beyond judgement-free communication, people need to get tested … whether you identify as at-risk or low-risk, it’s so important to get tested,” Tivey says.