News
Teen Girls Would Pay The Ultimate Price Under The AHCA
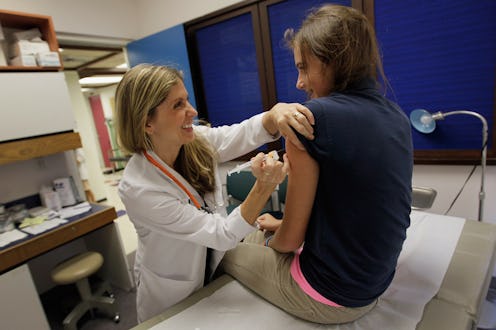
Since narrowly passing in the House of Representatives last week, the American Health Care Act has been assailed by critics from numerous angles. Democrats have accused Republicans of simply crafting a tax cut for the rich while cutting health care for the rest of Americans, and strangely enough, some conservatives are almost agreeing.
One of the most prominent aspects of the health care bill is the $880 billion cut to Medicaid, along with changes to the program which would force states to cap their spending at certain levels. It stands in contrast to the current system, in which Medicaid covers all health care needs of its enrollees. While much of the discussion and criticism of the AHCA has been around what it will mean for the elderly — and those are certainly legitimate — the cuts to Medicaid would also have a large effect on children and teenagers. Medicaid covers around 37 million children around the United States, according to the Georgetown University Health Policy Institute.
Cuts to that program could be especially devastating to young girls who get their health care through it. "Medicaid is already a very lean program. It spends less per capita on average than private plans," Elisabeth Burak, Senior Program Director at the Center for Children and Families at Georgetown University, tells Bustle. "There isn't a lot of fat to cut in Medicaid as it is, so with over half of Medicaid recipients being kids, it's hard to imagine they wouldn't be affected."
Kids are the cheapest group of people to cover under Medicaid, but with them being forced to compete with other groups — seniors in nursing homes, poor people who need the assistance — Burak worries that they could nevertheless lose funding and access to care if total Medicaid spending was capped. "Even states that want to do the right thing for kids might be forced to cut back in terms of eligibility or services or payment because they just don't have enough money in the system," she says.
For young girls, that may mean less access to some critical care. According to Lara Kaufmann, Director of Public Policy at Girls Inc., a mentoring and advocacy organization for young girls, adolescent women face specific health care needs relating to sexual abuse, reproductive health, and mental health counseling. All three of those could be affected by changes in regulations under the American Health Care Act.
Medicaid is a really smart investment in kids... Beyond just their health, though their health is certainly important. But it also sets them up for success later in life too.
Before the passage of the Affordable Care Act in 2010, complications from sexual assault (such as STI treatment and counseling) could be counted as preexisting conditions used to deny treatment. Under the AHCA, states could potentially allow insurers to charge patients more for these kinds of complications if the patient has been lapsed in coverage for more than 63 days and purchases insurance on the individual market. While the higher premium would only be for a year in this situation, it could still pack a financial punch. With one out of four girls experiencing sexual abuse before the age of 18, according to the National Child Traumatic Stress Network, this could hit young girls hard.
Similarly, the need for mental health counseling is especially high among adolescent girls. According to Kaufmann, 80 percent of teenage girls who end up involved with the justice system show some type of mental health diagnosis, often from trauma. Under the Affordable Care Act, all health plans are required to include mental health coverage, but the new health care act allows states to no longer require that of plans.
Our strong belief for our girls is that they're entitled to education, informed decision-making, and what they need to make the choices that are right for them... So, we want that health information and services to be readily available and accessible to all women and girls.
And of course, teenage girls face a threat from the provision of the bill that denies Medicaid funds from paying for any services at women's health clinics that perform abortions (most notably, Planned Parenthood). Low-income women can be especially reliant on Planned Parenthood and other similar women's health providers, and losing the ability to use Medicaid to pay for contraceptive care, STI prevention, or maternity care at those clinics could make reproductive health more difficult.
Beyond that, according to Kaufmann, a major part of reproductive health coverage for young girls comes in the form of sexual education, which clinics like Planned Parenthood include as part of their mission. "Our strong belief for our girls is that they're entitled to education, informed decision-making, and what they need to make the choices that are right for them," she tells Bustle. "So we want that health information and those services to be readily available and accessible to all women and girls."
The effects of affordable access to good health care for young girls doesn't just affect them in the present. According to a study from the Center for Children and Families at Georgetown University, bringing children on to Medicaid in the 1980s led to improved outcomes for education and economic well-being as adults — more likely to graduate high school and college, and more likely to earn more in their jobs.
"Medicaid is a really smart investment in kids," says Burak. "Beyond just their health, though their health is certainly important. But it also sets them up for success later in life too."