Life
7 Things To Know About Getting An IUD
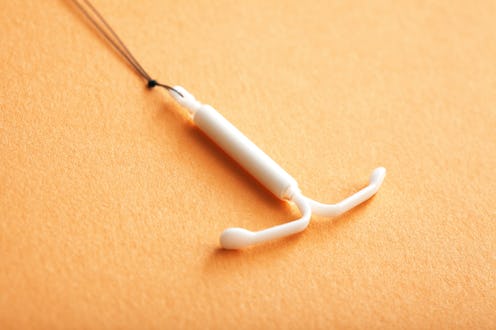
Before president-elect Donald Trump officially takes office in January, women on Twitter are encouraging each other to seriously consider their birth control options, before he makes them harder to access. (He's said he'd repeal the Affordable Care Act, which gives women free birth control). While some have suggested to stock up on Plan B and other forms of hormonal birth control while you can (keep in mind those have expiration dates), a ton of women are also speaking up on long-acting birth control options such as intrauterine devices (IUDs). According to an ABC News report, Google searches for IUDs have “spiked exponentially” in the hours after the election was called. It’s so great to see women fighting back by taking control over their bodies and reproductive health — something which many women fear will be taken away in Trump’s America. Getting an IUD now more than ever seems like the best possible thing. So, what are some things you should know about getting an IUD?
"The major advantages of an IUD are the fact that the device is more effective than oral contraceptive pills," Dr. Gil Weiss, Assistant Professor of Clinical Medicine at Northwestern Memorial Hospital and partner at the Association for Women's Health Care tells Bustle. "In fact, less than one in 100 women will get pregnant using an IUD. Additionally, the device is not dependent on human behavior (i.e. remembering to take a pill or using a condom appropriately). I always like to say that IUDs are low maintenance birth control for these reasons."
The IUD is nothing new. According to a UN analysis from 2010, 15 percent of the birth control using world uses IUDs. It’s actually the second most commonly used form of birth control overall. “I insert IUDs almost daily in my practice and I’m a big fan,” Sara Twogood, MD, FACOG, Assistant Professor of Clinical Obstetrics and Gynecology at the Keck School of Medicine at the University of Southern California tells Bustle. “Almost anyone is a candidate for an IUD. However women with a uterine anomaly (such as a bicornuate uterus or large fibroids) are not generally good candidates.”
So it is popular, but judging how the conversation over the IUD has grown like crazy over the past 24 hours, it seems like there’s still so much out there women need to know. For some time now, there's been a big push towards LARC contraception (long acting reversible contraception) since they're more effective at preventing unwanted pregnancy than short acting forms. Getting an IUD placed essentially protects a woman for three to 10 years depending on the type of IUD. She can make the conscious decision that she is ready to attempt pregnancy and have it removed, as opposed to remembering on a day to day basis to take a pill to prevent an unwanted pregnancy. "I tell women that the procedure is minor, I do it all the time, and it is quick. If a woman is particularly anxious, I may prescribe her an anxiolytic to take before the procedure itself," Twogood says.
If you’re deciding what to do about the future of your birth control, here are some things you should know about getting an IUD:
1. There Are 2 Options: Hormone-Free (Paragard, The Copper IUD) And Levonorgestrel-Containing IUD (Mirena Or Skyla)
According to Twogood, Skyla is the only one that’s FDA approved for nulliparous women, meaning women who have never been pregnant. But Mirena and Copper IUDs can also be safely used. This is important to note because a common misconception about IUDs is that it’s only for women who’ve been pregnant before. But as Twogood says, it’s not true.
“This misconception is based on the studies to get the IUDs approved through the FDA,” Twogood says. As the story goes, the original Mirena study used multiparous women, or women who have previously had a baby. So when it was FDA-approved, it was FDA-approved for women they studied. But that doesn't mean it can't be used for women who’ve never been pregnant before.
“Large studies have shown it's safe for these women. It's just not FDA-approved for them, so technically it's an ‘off-label use,’” Twogood says. “The pharmaceutical industry has corrected this misconception with Skylab which is marketed as ‘Mirena's little sister.’ It is FDA-approved for nulliparous women, intentionally. They made it slightly smaller and with a lower dose of progesterone, and intentionally used nulliparous women in the FDA approval studies. I'm still using Mirena for any woman who wants a hormonal IUD. Bleeding is better with Mirena and the benefits of keeping it on for five years instead of three is also preferred.”
2. Despite What You May Have Heard, IUDs Don’t Increase The Risk For Pelvic Inflammatory Disease (PID)
In the first 21 days after insertion, the risk for PID is increased IF you already have a preexisting infection. “This is why I first schedule an exam to look for any signs or symptoms of an infection before inserting the IUD,” Twogood says. “ After 21 days however, the IUD is protective against PID.”
3. It Won’t Affect Future Fertility
I think anytime you play around with birth control options, the question over what it might end up doing to your reproductive system will come up. But according to Twogood, the levonorgestrel (progesterone) in Mirena “acts locally.” Meaning, a small amount is absorbed systemically, but not enough to stop ovulation.
“When any IUD is removed, studies show us that she can get pregnant immediately (versus the delay women experience with birth control pills and Depo-provera),” Twogood says. “A rare complication of an IUD is scarring inside the uterus. If a woman develops an inflammatory response to the IUD (or develops PID), this could lead to scarring. This outcome could affect future fertility but it is very rare and is even more unlikely if precautions are used.”
4. Your Partner Shouldn’t Feel It When You Have Sex
During heterosexual sex, some men may feel the IUD strings, but it’s usually not something to worry about. Doctors usually know to trim the strings so that the ends don’t stick outside of the cervix.
5. There Are Side Effects
Side effects like acne, depression, and mood swings are real, do happen, and are not very well publicized with hormonal IUDs. “They are also not common,” Twogood says. “I wouldn't suggest against a Mirena for these concerns, but I also counsel my patients about the possibility, so if they experience these side effects they know not to disregard them.”
6. The Procedure Is Simple, But Can Be Uncomfortable
Getting a procedure may seem scary. Some women may find it excruciatingly painful and some women may breeze through the entire thing. As Twogood says, “It’s pretty unpredictable.” The procedure itself goes like this:
- A speculum is inserted and the vagina and cervix are inspected for any signs of infection like chlamydia or bacterial vaginosis.
- If no signs of infection are present, the cervix is cleaned with a cool liquid (usually betadine). Some practitioners may even place an instrument called a tenaculum on the cervix to help stabilize it. Practitioners may also use an instrument called uterine sound to get an idea of the size and shape of the uterus before inserting the IUD.
- If everything looks good, the IUD is then inserted through the cervix and inside the uterus.
- Once released inside the uterus, all instruments are removed and the strings are then trimmed.
“The patient can expect some cramping pain and discomfort for several hours afterwards, but it's not expected to get in the way of day to day activities. I also suggest women take ibuprofen before the procedure to help minimize the discomfort,” Twogood says.
Personally, I’ve never had an IUD. I’m actually in the same boat as many women out there who’s seriously considering one. And it seems like the procedure isn't too bad.
“The overall procedure was actually pretty seamless and I really have my roommate to thank for this," Selena Yang, the PR Manager of Progyny, a company dedicated to providing fertility solutions to employers and individuals, tells Bustle. "Her advice was to take ibuprofen before the procedure and she walked me through the type of pain I would feel—it’s this weird internal pain that we both can’t describe—and how I could cramp a few days later. Naturally I re-asked my gyno all the same questions. During the procedure, my gyno talked about each step as it was happening which was great. The procedure itself didn’t last that long. I didn’t really experience too much cramping, just slight, and the rest is history. It’s only been a few weeks, but I’m really glad I got it! It’s actually pretty freeing not having to worry about taking a pill every morning.”
7. Here Are Some Other Things To Know About The Procedure
The entire process should take about five minutes for the insertion. It doesn’t require anesthesia. While the insertion can be painful and make you feel crampy like you’re on your period, women of all ages, regardless of whether or not they have had children already, say they tolerate the insertion very well. If not, you can always take over the counter pain medicine about 30 minutes before the insertion which can really help with the pain and cramps you may experience. After insertion you can go about your day like normal. So there’s really no need to take a day off from work or anything. Unless you really want to.
“I think the best candidate for the IUD are women who do not want to get pregnant for at least the next two years,” Dr. Fahimeh Sasan, Consultant Medical Doctor at Progyny and OBGYN at Mount Sinai tells Bustle. “It's a great form of contraception because it doesn’t require you to do anything—once the doctor places the IUD you are all set. For example: You don't have to remember to take a pill daily, or remove your Nuvaring after 21 days, or go for a Depo Provera injection every three months. For women who medically need or personally want a non-hormonal form of contraception and do not want to use condoms, the copper IUD is ideal.”
I know the future of your reproductive rights seems pretty daunting now that Donald Trump is the president-elect. Who knows what 2017 is going to look like. I’m so glad many women are taking the necessary steps to take care of themselves. While IUDs seem like the best option since it is long-acting, I wouldn’t suggest you run out the door and get one ASAP. Like any other form of birth control, it’s important to weigh the pros and cons, think about your medical history, and of course, discuss it with your doctor.
Images: Image Point Fr/Shutterstock; Giphy