Health
What Happens To Your Body If You Get The Vaccine After Having COVID
Whether you had a mild case or have long-haul symptoms still, getting vaccinated will help end the pandemic.
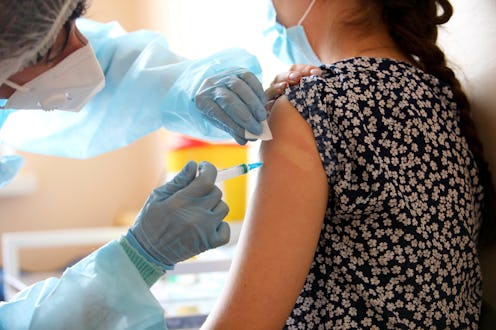
With a host of COVID-19 vaccines now cleared for emergency use by the FDA, the vaccination program against the Virus That Completely Ruined 2020 is fully underway. If you’re one of the estimated 30 million or so Americans who’ve had COVID, whether in the past three weeks or last year, you may be wondering what getting the vaccine will mean for you. Do people who’ve had COVID need to get the vaccine, since they should have antibodies to fight off future infections? What if you’re still dealing with long-haul COVID?
Can You Get The COVID Vaccine After Having COVID?
The big takeaway is that, yes, anyone who’s had COVID should still plan to get the vaccine to be maximally protected against future infections. Having a previous case of COVID doesn’t mean the vaccines will be any less effective. In fact, two small preprint studies published in 2021 suggested that people who’ve had COVID may only require one dose of an mRNA vaccine to be fully protected, though further research is needed. People who’ve previously had COVID will be as well-covered against future illness as everybody else who gets jabbed.
“We recommend the vaccine for all those who are eligible, even those who have long haul symptoms and with prior COVID,” Dr. Monica Lypson M.D., co-director of the COVID-19 Recovery Clinic at the George Washington University Medical Faculty Associates, tells Bustle.
When To Get The COVID Vaccine After Being Sick
If your COVID case was recent, however, you should sit tight. “In general, we are recommending that after a diagnosis of COVID, people wait 90 to 120 days before getting the vaccine,” she says.
Waiting serves two purposes, Dr. Teresa Bartlett M.D., senior medical officer at claims management company Sedgwick, tells Bustle. “First, you have some antibodies in your system for a period of three to six months,” she says. That means the vaccine might not actually be necessary yet, and other people should be prioritized in the vaccine queue. After that period, though, your natural antibodies will have faded, and the vaccines are designed to produce more robust, lasting immune protection over time.
Dr. Bartlett says she’s also seen people who’ve had recent COVID have a reaction to the vaccine if taken too soon. The ZOE COVID Symptom Study found that people who’d had COVID previously were nearly twice as likely to experience mild reactions to the Pfizer vaccine, compared to people who’d never tested positive for COVID. “This is because many have already mounted an immune response, so they are primed to recognize the SARS-CoV-2 spike protein that the mRNA instructs our cells to make,” Dr. Natasha Bhuyan M.D., regional medical director for One Medical, tells Bustle. Waiting a few months after your COVID has subsided means your immune system will calm down and be less likely to respond so vigorously to vaccines.
Why The COVID Vaccine Could Help Some Long-Haulers’ Symptoms
People who have long-haul COVID, with persistent symptoms like fatigue, headaches, or shortness of breath lasting for months after their initial bout, may have heard that the vaccine could help them feel a bit better. “There are some emerging reports of some patients’ symptoms improving after vaccination,” Dr. Hana Akselrod M.D., a fellow co-director of the George Washington University COVID-19 Recovery Unit, tells Bustle.
Dr. Akselrod says that while the science on this is very new, there are a few interesting theories about why COVID long-haulers could feel better after their vaccines. “Conceptually, there is a possibility that vaccination helps turn a disorganized or ‘misfiring’ immune response to SARS-CoV-2 into a more efficient and directed one,” she says.
Yale University professor of immunology Akiko Iwasaki suggested in a Medium article that people with long COVID might have a combination of three different issues: a persistent low-level virus, fragments of the initial virus’s DNA hanging around in the bloodstream, or an autoimmune response. The COVID vaccine can theoretically help all three issues, by eliminating the low-level virus and the DNA fragments, and helping the body retrain its immune responses to be more effective. Harvard Health notes there are other theories about long-haul COVID symptoms that need to be tested too, including brain inflammation or problems with the autonomic nervous system, which regulates things like your digestion and heart rate. Without more information about what causes long-haul COVID, it’s hard to pinpoint how vaccines might affect people with the condition.
But Dr. Akselrod emphasizes that individual responses to the jabs will probably vary. “Long COVID is likely not a singular process for everyone — some people may feel better, while others feel the same, or experience side effects from the vaccine.”
People who’ve had long COVID might want to wait until their symptoms lull before booking a vaccine appointment, Dr. Lypson says. “We might recommend waiting until they are closer to their baseline than not,” she says. “The vaccine may cause an exacerbation of their symptoms for a short period of time.” But Dr. Akselrod says everybody should still get the shot, because catching the infection a second time will likely be worse than any temporary side effects of the vaccine.
Experts:
Dr. Hana Akselrod M.D.
Dr. Teresa Bartlett M.D.
Dr. Natasha Bhuyan M.D.
Dr. Monica Lypson M.D.
Studies cited:
Krammer, F., Srivastava, K,. PARIS team, Simon, V. (2021) Robust spike antibody responses and increased reactogenicity in seropositive individuals after a single dose of SARS-CoV-2 mRNA vaccine. MedRxiv [Preprint]. https://www.medrxiv.org/content/10.1101/2021.01.29.21250653v1
Saadat, S., Rikhtegaran-Tehrani, Z., Logue. J., et al. (2021) Single dose vaccination in healthcare workers previously infected with SARS-CoV-2. MedRxiv [Preprint]. https://www.medrxiv.org/content/10.1101/2021.01.30.21250843v2