Life
7 Myths About Lyme Disease Doctors Want To You To Stop Believing
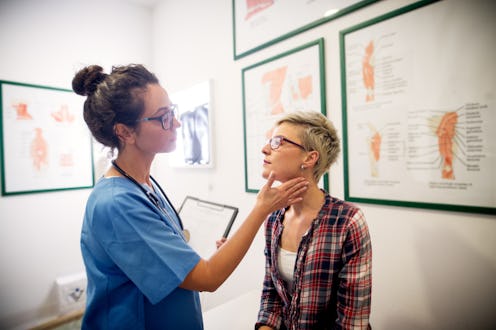
Tick-borne illness is spreading across the U.S.; the number of counties reporting Lyme disease infections has increased from 324 in 2008 to 415 in 2018, according to the Centers for Disease Control & Prevention (CDC). In 2018, over 33,000 people had confirmed cases. Yet even as more and more people become infected, many myths about Lyme disease prevent them from getting the proper diagnosis and treatment. Fortunately, we're starting to emerge from the dark ages, understand how the disease operates, and offer more compassion and empathy to the people suffering from it.
Some of the biggest myths about Lyme involve how it's diagnosed. "Individuals with Lyme disease expect a tick bite, bull’s eye rash, a positive Lyme disease test, and a good outcome after 21 days of antibiotics and no chronic illness," Dr. Daniel Cameron M.D. M.P.H , an internist and epidemiologist who specializes in treating Lyme, tells Bustle. "Instead, they often don’t see the tick bite, the rash is absent or atypical, the tests are not reliable, and they may not get better after 21 days of antibiotics."
Because Lyme is so prevalent, it's important to learn accurate information about it so that you can spot it in yourself and support loved ones who may contract it. Here are some myths about Lyme that are in desperate need of clearing up.
Myth #1: If You Don't Remember A Tick Bite, You Don't Have Lyme
Not everybody remembers getting Lyme. Some people harbor it for years and keep it latent until a stressful situation triggers it to come out, Dr. Kristin Reihman M.D., family medicine doctor and author of Life After Lyme, tells Bustle.
"In today’s world of high stress, environmental man-made contamination, genetically modified foods, imbalances in the check-and-balance of species both internally and externally, well this can culminate to be the triggering event for someone’s system to break down," Mary-Beth Charno, APRN-C, a nurse practitioner who specializes in treating Lyme, tells Bustle.
Furthermore, Lyme is not always caused by tick bites. "Borrelia Burgdorferi has been found in all sorts of biting insects [like] fleas [and] mosquitos," says Dr. Reihman. "It's also found in human breastmilk and semen and in placentas of miscarried babies, so there are lots of ways Lyme can be transmitted."
Myth #2: If You Didn't Get A Rash, You Don't Have Lyme
Many doctors will diagnose Lyme based on the presence of a rash shaped like a bull's eye, but only nine percent of Lyme patients get one, according to Lymedisease.org. If you don't get a rash, this is often a sign that your immune system is down. "The rash is a function of a robust immune response," says Dr. Reihman. "So if you do remember a rash, chances are your immune systems is doing a lot more work than someone who doesn't. A rash shows up if the immune system comes to do its work. I'm more concerned about someone who doesn't get a rash than someone who does."
Myth #3: If You Tested Negative, You Don't Have Lyme
The Western Blot and ELISA, the tests most commonly given to patients suspected to have Lyme, produce many false negatives, says Dr. Reihman. A study published in The American Journal of Medicine in 2017 also found that, because it takes several weeks for antibodies to develop, many patients with Lyme disease will test negative early on in the illness, and then test positive later on.
Not all doctors know how to deal with Lyme, either. "Testing for Lyme is sometimes challenging for physicians not completely familiar with the infection," Dr. Andres Romero M.D., an infectious disease specialist at Providence Saint John Health Center, tells Bustle. "Advice from an infectious disease physician is recommended."
The International Lyme and Associated Diseases Society recommends that doctors make "a clinical diagnosis based on the history and physical findings, and supported by appropriate laboratory tests when they are indicated." In other words, you can be diagnosed based on your symptoms even without positive test results.
Myth #4: You Can Only Get Lyme In Certain Geographical Areas
Some people with Lyme symptoms assume they don't have Lyme because they don't live in Lyme endemic areas like the U.S. northeast. But in reality, nearly everyone is susceptible to it. "Lyme has actually been found in all 50 states and most countries," says Dr. Reihman. "It can really go anywhere."
Myth #5: Lyme Disease Heals Up After Antibiotics & Never Comes Back
Despite celebrities from Yolanda and Bella Hadid to Avril Lavigne speaking out about their experiences with persistent Lyme disease infections, coverage often describes the diagnosis as "controversial."
"Chronic Lyme disease is complex and often misunderstood, which means that many patients will struggle to obtain the care they need to regain their health," says Charno.
Infectious disease experts will often use the term post-treatment Lyme disease syndrome (PTLDS) to refer to a case where symptoms of documented Lyme disease — like aches, brain fog, joint pain — continue after treatment and become chronic. Around 5-20% of patients with Lyme disease will go on to have chronic symptoms, per the Lyme & Tick Borne Diseases Research Center at Columbia University Irvine Medical Center, and the chances of having a chronic infection go up the later Lyme is diagnosed and treated.
"Chronic illness is not disputed in numbers of other health challenges," says Charno. "We don’t say that all congestive heart failure will resolve with treatment, or that once diabetes is adequately treated, that it doesn’t persist for some. Why is this concept so difficult to apply to tick illness?"
Myth #6: Lyme Looks The Same For Everyone
"Borrelia burgdorferi has 132 lipoproteins," Charno says. "These lipoproteins are pro-inflammatory, they modulate immunity, and they enable the spirochete to evade the immune system. Depending on many factors, people will present vastly differently in how the inflammation shows up."
Lyme "can impact any organ system or tissue of the body," Dr. Reihman says. This means that it can cause a wide variety of symptoms, and they're not the same for everyone.
Another reason Lyme presents itself in so many different ways is that there are different Borrelia species that can cause it, and the Borrelia carries co-infections that are different in different patients. For example, some may primarily have Bartonella in their system, while others are experiencing symptoms of Babesia.
All You Need To Kill Lyme Is A Few Weeks Of Antibiotics
Doctors typically treat early Lyme with 28 days of the antibiotic Doxycycline. While this does work in some cases, it doesn't work in others. "People have Lyme that persists after 28 days, but because of this myth, they're often denied further treatment," says Dr. Reihman. Because there are often stressors in someone's physical surroundings or personal life that keep the illness around, treatment also involves reducing stress, optimizing sleep, staying away from environmental toxins, and supporting the body's functioning, she says.
If you think you might have Lyme Disease, you can assess your symptoms by filling out the Horowitz Lyme-MSIDS Questionnaire and find a Lyme-literate doctor who can help determine how to treat your symptoms.
Experts:
Dr. Daniel Cameron, M.D., M.P.H.
Mary-Beth Charno, APRN-C
Dr. Kristin Reihman, M.D.
Dr. Andres Romero, M.D.
Studies cited:
Kenedy, M. R., Lenhart, T. R., & Akins, D. R. (2012). The role of Borrelia burgdorferi outer surface proteins. FEMS immunology and medical microbiology, 66(1), 1–19. https://doi.org/10.1111/j.1574-695X.2012.00980.x
Middelveen, M. J., Sapi, E., Burke, J., Filush, K. R., Franco, A., Fesler, M. C., & Stricker, R. B. (2018). Persistent Borrelia Infection in Patients with Ongoing Symptoms of Lyme Disease. Healthcare (Basel, Switzerland), 6(2), 33. https://doi.org/10.3390/healthcare6020033
Shapiro, E.D., Baker, P.J., Wormser, G.P. (2017) False and Misleading Information About Lyme Disease. Am J Med. 130(7):771-772. doi: 10.1016/j.amjmed.2017.01.030. Epub 2017 Feb 16. PubMed PMID: 28216447.
This article was originally published on