Health
5 COVID-19 Testing Myths, Debunked By A Doctor On The Frontlines
Your results are only accurate to the moment you got swabbed.
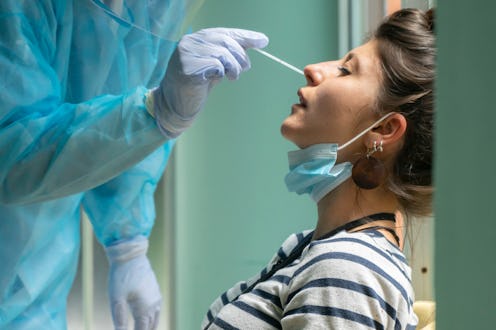
After many months of testing shortages, delays, and restrictions on who can be tested, COVID-19 testing in the U.S. has become more available to symptomatic and asymptomatic patients alike. Still, there are a lot of myths about coronavirus testing and what the results indicate.
According to internist Dr. Sunitha D. Posina, M.D., people have become a little too quick to think that testing negative for the virus, or testing positive for the antibodies, means that they are free to mingle and throw caution to the wind. "A lot of people are getting mixed information about COVID-19 testing and the various interpretation of the results." Dr. Posina worked on the frontlines of the coronavirus crisis in New York, managing the treatment of COVID patients that were admitted to the hospital. "During those few months (from March to June), I would at maximum see one or two patients that didn't have COVID-19; the rest of the patients I was treating were all COVID-19," she says. Though the situation has improved since those early days, it's important to really understand what your test results do and don't mean, so you don't accidentally put someone else at risk.
Here are a few coronavirus testing myths, and the reality behind them.
1Myth 1: If Your COVID-19 Test Results Are Negative, You Are Still Negative, No Matter When You Got Your Test.
When you get your test results, they will mirror your state of health at the time of the test, not at the present. If you got a rapid coronavirus test at a hospital, your results — positive or negative — are accurate as of 15 minutes ago. If you took a test at an urgent care and it took over a week to get results back, as some places in the country are reporting, your results are only accurate as of a week ago. And if you were exposed to coronavirus since then, your results are no longer up to date.
To ensure that your results are actually applicable, take all protective measures (face mask, hand-washing hygiene) and quarantine once you leave your doctor's office. "Otherwise, the test results would be void, and you still have a risk of contracting a new infection on your way out of the office if proper social distancing measures are not maintained," Dr. Posina says.
2Myth 2: All Coronavirus Tests Are The Same
There are two types of tests that are done to detect an active coronavirus infection. One is an RT-PCR (Reverse transcriptase – Polymerase Chain Reaction), aka PCR, and the other one is a viral antigen test.
The PCR test is considered the "gold standard" because it can detect even subtle traces of the virus. Dr. Posina explains that because this test can find any genetic material evidence of the virus, it's more thorough than any other test currently available. For this test, the sample swab is usually obtained from the nose or throat and can take a few days or up to a few weeks to get results, depending on how backed up the lab is. It's nearly 100% accurate if performed correctly.
The viral antigen test looks for viral surface proteins to detect the infection, and also relies on a sample from the nose or throat. While this test is more affordable, and offers faster results, it's less accurate. "They have about 20% to 30% false-negative results because one needs to have significant amounts of viral proteins for the test to detect it," Dr. Posina explains.
There's also a blood test, called the Serology Antibody test, which determines if you had a past infection. Dr. Posina says that all an antibody test can tell you is that the illness you had was indeed COVID. Scientists think having antibodies means you should be protected from getting COVID again, but it's still not clear how long that protection lasts, if at all. Meaning, a positive antibody test doesn't mean you can ditch your mask, go to a party, or behave any differently than if you didn't have the antibodies.
3Myth 3: You Don't Have To Completely Isolate After Getting Tested
Not following social distancing protocols defeats the purpose of being tested. According to Dr. Posina, you can easily get infected with COVID on your way out of the testing facility if you pass a sick patient or touch an infected door, then touch your face. "If you come in contact with someone that has an active infection on your way out of the office, whether they are symptomatic or not, puts you at risk of contracting it from them if you didn't have it while you were getting tested."
Dr. Posina says it's incredibly important to avoid touching your face, to steer clear of other patients, and to sanitize your hands after touching anything, especially while in a doctor's office. But what's more, you'll need to keep up with this level of hygiene and isolation until the results come to ensure your results stay accurate. The subtext here is that if you follow all recommended protocols and get a negative result, that doesn't mean you can go hug a friend or throw a party. To stay negative after establishing the COVID-free baseline, you've got to stay safe.
4Myth 4: You Can Get Tested Any Time After Getting Exposed
It takes a few days for the virus to become present enough in your system to be detected. If you test too soon after potentially being exposed, you could get a false negative result.
"The incubation period of the virus is anywhere from four to 14 days, and most of the people have been developing symptoms around five to six days into the infection," Dr. Posina says.
"My best educational guess would be to get tested sometime around the seventh or eighth day unless someone develops significant severe symptoms such as shortness of breath, chest pressure, new onset of confusion," she adds.
According to Harvard Health, a person might become symptomatic and contagious after only 48 to 72 hours from exposure, so talk to your doctor about the best time to test, based on your individual experience. According to a John Hopkins study, people who tested within four days of infection are 67% more likely to test negative even if they had the virus, so if you don't have symptoms, and you can wait to test, you should.
5Myth 5: If You Don't Have Symptoms, You Don't Need To Get Tested
If you think you might have been exposed to someone with COVID-19, get tested. Dr. Posina says that there's no value in "saving a test" because you're already planning to isolate, though you should be isolating too. Not only is it important to ensure that coronavirus tracking is as accurate as possible — if you are sick, you should be accounted for — but finding out your status is also crucial for contact tracing. If you test positive, you and a contact tracer can get in touch with everyone you've come into contact with and let them know they may be at risk. This is critical to curb the spread of the virus.
Expert:
Dr. Sunitha D. Posina MD, a board-certified physician of Internal Medicine in Stony Brook, New York.
Study cited:
Kucirka, L., Medicine, J., Lauer, S., Johns Hopkins Bloomberg School of Public Health, Laeyendecker, O., Boon, D., . . . M. Centor, R. (2020, June 16). Variation in False-Negative Rate of Reverse Transcriptase Polymerase Chain Reaction–Based SARS-CoV-2 Tests by Time Since Exposure. Retrieved August 18, 2020, from https://www.acpjournals.org/doi/10.7326/M20-1495
This article was originally published on